Understanding the Physical Toll of Withdrawal: Why Medical Detox is Essential for Safety.
physical toll Addiction is a complex, multifaceted condition that affects millions worldwide. Breaking free from substance dependence is often the first step toward recovery, but the process of withdrawal—the body’s response to the abrupt cessation of a substance—can be perilous. Withdrawal is not merely uncomfortable; it can be life-threatening. Understanding its physical toll is critical for anyone navigating recovery, whether personally or for someone they care for. This blog post explores the physiological challenges of withdrawal, breaks down the risks associated with different substances, and explains why medical detox is vital for safety and long-term healing.
The Physical Toll of Withdrawal
When the body becomes dependent on a substance, it adapts by adjusting its chemistry. Sudden discontinuation triggers a cascade of compensatory reactions, leading to withdrawal symptoms. These symptoms vary in intensity and duration, depending on the substance, the duration of use, and individual physiology. Below is a detailed breakdown of the physical toll of withdrawal for common substances:
| Substance | Common Withdrawal Symptoms | Withdrawal Timeline | Potential Complications |
|---|---|---|---|
| Alcohol | Tremors, insomnia, sweating, nausea, anxiety, increased heart rate, hallucinations | 6–48 hours after last drink; peaks at 24–72 hrs | Delirium tremens (severe confusion, hallucinations), seizures, cardiovascular collapse |
| Opioids | Muscle aches, diarrhea, vomiting, insomnia, sweating, agitation, cold flashes, dilated pupils | 6–30 hours (short-acting); 12–48 hours (long-acting) | Severe dehydration, electrolyte imbalance, heart palpitations, suicidal ideation |
| Benzodiazepines | Anxiety, insomnia, tremors, irritability, muscle cramps, paranoia, seizures | Begins 6–12 hours; peaks at 72 hours | Status epilepticus (prolonged seizures), psychosis, cardiac arrhythmias |
| Stimulants (Cocaine, Methamphetamine) | Fatigue, depression, increased appetite, vivid dreams, insomnia, paranoia | 24–72 hours | Cardiac events (e.g., heart attack), severe depression, suicidal thoughts |
| Nicotine | Irritability, stress, difficulty concentrating, cravings, insomnia, increased appetite | Peaks within 2–3 days; lasts weeks | Elevated risk of smoking relapse, persistent cravings |
| Barbiturates | Confusion, seizures, agitation, sweating, respiratory depression | 6–12 hours | Seizures, coma, respiratory failure |
| Cannabis | Insomnia, irritability, poor appetite, anxiety, restlessness | 2–3 days; lasts 7–21 days | Rare but possible mood disorders (e.g., depression, psychosis) |
Key Takeaway: While some symptoms are manageable, others—like alcohol withdrawal seizures or benzodiazepine-induced seizures—can be fatal without medical intervention. This table underscores the urgency of addressing withdrawal in a supervised setting.

Why Medical Detox is Essential
1. Mitigating Life-Threatening Risks
Certain withdrawal processes are inherently dangerous. For example, alcohol withdrawal can lead to delirium tremens (DTs), a medical emergency with a 5–25% mortality rate if untreated. Similarly, abrupt cessation of benzodiazepines can trigger status epilepticus, a seizure disorder that may cause permanent brain damage or death. Medical detox centers are equipped to handle these crises with medications like lorazepam to prevent seizures and benzos to manage DTs.
2. Managing Withdrawal Symptoms Effectively
Medical professionals use evidence-based protocols to alleviate symptoms:
- Alcohol: Benzodiazepines (e.g., diazepam) to control seizures and anxiety.
- Opioids: Medications like methadone, buprenorphine, or clonidine to ease cravings and discomfort.
- Stimulants: Beta-blockers to manage elevated heart rates and blood pressure.
Example: A 2019 study in The New England Journal of Medicine found that patients undergoing opioid detox with buprenorphine had 70% fewer relapse rates compared to those without medication support.
3. Preventing Dehydration and Nutritional Deficiencies
Withdrawal often causes gastrointestinal distress (vomiting, diarrhea), leading to electrolyte imbalances. In severe cases, this can result in heart arrhythmias or kidney failure. Medical detox programs monitor hydration levels and administer IV fluids if needed.
4. Tailoring Care to Individual Needs
Substance use disorders often co-occur with mental health conditions (e.g., depression, PTSD). Medical detox teams assess patients holistically, adjusting care plans to address these complexities.
Factors Influencing Withdrawal Severity
- Duration and Dosage of Use: Longer use and higher doses increase dependency, leading to more severe symptoms.
- Method of Use: Smoking or injecting substances may result in harsher withdrawal due to higher bioavailability.
- Co-occurring Conditions: Anxiety, depression, or chronic illness can exacerbate withdrawal symptoms.
- Genetics and Biology: Genetic predispositions affect how the body metabolizes substances.
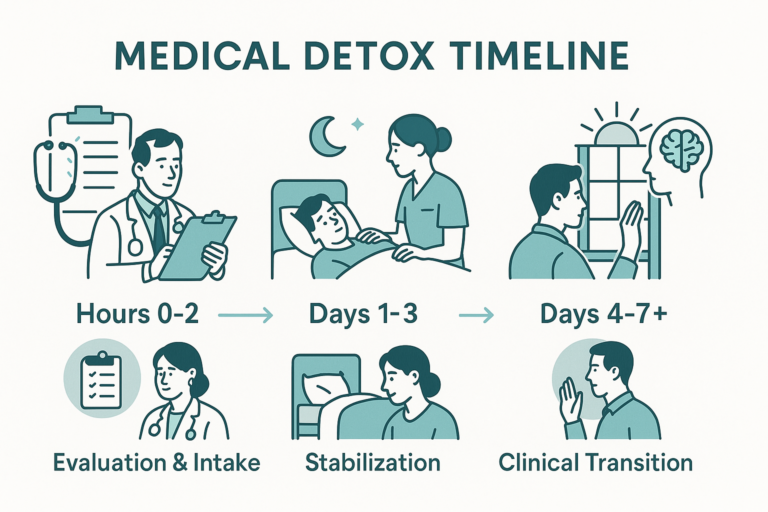
The Medical Detox Process
Medical detox is not a standalone solution but the first step in recovery. Here’s what it typically entails:
- Assessment: Physicians conduct physical and psychological evaluations to create a personalized plan.
- Monitoring: Vital signs (heart rate, blood pressure, temperature) are tracked 24/7.
- Medication Management: Symptom-specific medications are administered gradually to stabilize the patient.
- Supportive Care: Nutritional therapy, hydration, and counseling help address both physical and emotional needs.
Aftercare and Long-Term Recovery
Detox is only the beginning. Long-term recovery requires:
- Inpatient/Outpatient Rehabilitation: Structured programs addressing the root causes of addiction.
- Therapy: Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), and group therapy.
- Support Networks: Programs like Alcoholics Anonymous (AA) or SMART Recovery provide community and accountability.
- Family Involvement: Loved ones can participate in education and counseling to foster a supportive home environment.
Conclusion
Withdrawal is a formidable challenge, but it doesn’t have to be faced alone. Medical detox provides the safety, expertise, and compassion necessary to navigate this critical phase. By understanding the physical toll of withdrawal and the risks of self-detox, individuals can make informed decisions that prioritize health and long-term recovery. If you or someone you love is struggling with addiction, reaching out to a medical detox center is the first—and most vital—step toward a healthier future.
Call to Action: For those seeking help, contact a licensed addiction treatment center today. Your journey to recovery begins with a single, empowered decision.
Sources & Further Reading:
- National Institute on Drug Abuse (NIDA)
- The American Journal of Psychiatry
- Substance Abuse and Mental Health Services Administration (SAMHSA) Guidelines

[…] barriers, and stigma. For individuals or loved ones seeking help, the journey to finding the right treatment center can feel overwhelming. However, evidence-based practices (EBPs)—treatment approaches supported by […]
[…] use or overdose—play a crucial role in breaking down stigma and building trust. For example, the eer Support Network in New Jersey ttrains former addicts to conduct naloxone workshops in their […]
[…] Why More People Prefer to Buy Weed Online […]