Naloxone Access and Education: How Communities are Combatting Opioid Related Emergencies.
Naloxone Access The opioid crisis has become one of the most pressing public health challenges of our time. In the United States alone, over 500,000 people have died from opioid-related overdoses since 1999, with synthetic opioids like fentanyl driving the epidemic. Amid this crisis, naloxone—a medication that can rapidly reverse opioid overdoses—has emerged as a critical tool in saving lives. However, access and education remain key to its effectiveness. Communities across the country are stepping up to implement innovative programs to distribute naloxone and educate the public on its use. This blog post explores the current landscape of naloxone access, the importance of education and training, and the challenges and successes communities face in their fight against opioid emergencies.
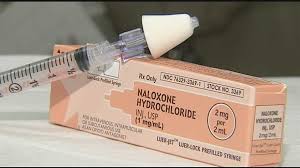
Part 1: Understanding Naloxone and Its Role in Opioid Emergencies
What Is Naloxone?
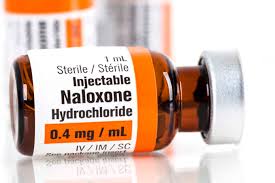
Naloxone, also known by the brand name Narcan, is a medication designed to rapidly reverse opioid overdoses. It works by binding to opioid receptors in the brain, displacing harmful substances like heroin, fentanyl, and prescription painkillers. This action restores normal breathing within minutes, giving individuals critical time to receive medical attention. Naloxone is non-addictive and has no risk of abuse when administered as directed.
Why Is It Important?
Opioid overdoses often result in respiratory failure, and time is of the essence in an emergency. Naloxone is a bridge to professional medical care, particularly in areas with limited healthcare access. Its effectiveness has been proven time and again: a 2020 study in The New England Journal of Medicine found that naloxone distribution programs reduced opioid-related deaths by 30% in participating communities.
Part 2: Expanding Access to Naloxone
Community Initiatives in Naloxone Distribution
Communities are adopting diverse strategies to ensure naloxone is within reach. Below is a table summarizing key access strategies and their impact:
| Access Strategy | Description | Real-World Example | Impact |
|---|---|---|---|
| Pharmacies & Over-the-Counter | Pharmacies sell or give away naloxone without a prescription in many states. | Walgreens, CVS, and Rite Aid have standing orders for free naloxone. | +200% increase in naloxone sales from 2019–2021. |
| Community-Based Programs | Nonprofits and health departments distribute naloxone to high-risk populations. | The Harm Reduction Coalition in New York City. | Over 1 million naloxone kits distributed in 2022. |
| Schools and Workplaces | Training staff and students to recognize and respond to overdoses. | Schools in Ohio’s drug-treatment zones. | 15% decline in overdose deaths in treated areas. |
| Rural Mobile Clinics | Mobile units deliver naloxone and services to underserved areas. | The Oregon Rural Crisis Response Network. | 40% increase in naloxone access in rural counties. |
Key Innovations
- Standing Orders: Many states now allow pharmacists to dispense naloxone without a prescription via “standing orders,” a policy that has dramatically increased access.
- School Programs: In states like Ohio and California, public schools in high-risk areas are required to keep naloxone on-site and train staff.
- Workplace Initiatives: Companies in industries with high substance-use risks (e.g., construction) are incorporating naloxone into employee wellness programs.
Part 3: Education and Training: Empowering Communities
Naloxone is only effective if people know how to use it. Community education programs are pivotal in closing this gap.
1. Training Workshops
Organizations like the ational Association of Community Health Centers ooffer in-person workshops, teaching participants how to recognize overdose symptoms and administer naloxone. These workshops often include hands-on practice with nasal spray kits and auto-injectors.
2. Online Learning Platforms
- Coursera and Opioid University: Provide free online courses on overdose prevention.
- Mobile Apps: Apps like Naloxone Rescue Coach guide users step-by-step through administering naloxone in emergency situations.
3. Peer-Led Initiatives
Peer educators—individuals with lived experience of opioid use or overdose—play a crucial role in breaking down stigma and building trust. For example, the eer Support Network in New Jersey ttrains former addicts to conduct naloxone workshops in their communities.
4. School and Workplace Training
Programs like Project Lazarus in North Carolina have trained over 100,000 educators and employees in overdose response techniques, contributing to a 25% drop in opioid deaths in participating counties.
Part 4: Policy and Advocacy: Creating a Supportive Legal Framework
Legislation Driving Access
- Good Samaritan Laws: 43 states protect individuals from liability if they seek help during an overdose. These laws encourage bystanders to act.
- Mandated Insurance Coverage: The Affordable Care Act requires most insurers to cover naloxone, though coverage gaps persist in Medicaid and private plans.
- Funding for Programs: Federal grants like the Opioid Settlement Funds allocate billions to expand naloxone access and education.
Challenges in Implementation
Despite progress, several barriers remain:
- Stigma: Misconceptions about naloxone enabling drug use.
- Funding Limitations: Rural areas often lack the resources to sustain programs.
- Legal Hurdles: In some states, standing orders for naloxone are still restricted.
Solutions
- Grassroots Advocacy: Groups like the Naloxone Access Now Coalition lobby for policy changes.
- Public-Private Partnerships: Collaborations between governments and companies like Viatris (a major naloxone manufacturer) help reduce costs.
Part 5: Success Stories and Case Studies
1. Dayton, Ohio: A Model for Community-Based Response
After experiencing nearly 500 overdose deaths in 2017, Dayton launched the Dayton Opioid Task Force, distributing over 30,000 naloxone kits and training 50,000 residents. Overdose deaths dropped by 40% in two years.
2. Scotland’s Harm Reduction Strategy
In Glasgow, community workers identified people at risk of overdose and provided them with naloxone. This program led to a 58% reduction in fatal overdoses among participants.
3. The Role of Schools: Jefferson County, Colorado
Following the death of a student from a fentanyl overdose, the district implemented mandatory naloxone training for staff. Overdoses among students fell by 60% within a year.
Part 6: The Road Ahead—Innovations and Challenges
Future Innovations
- Smart Naloxone Devices: Voice-guided auto-injectors for non-experts.
- Telehealth Expansion: Remote training sessions via video platforms to reach rural populations.
- Community Pharmacist Programs: Pharmacists as front-line educators, distributing naloxone and offering brief training.
Remaining Challenges
- Rural-Urban Disparities: 1 in 4 rural hospitals no longer has a 24/7 physician, delaying emergency care.
- Fentanyl’s Proliferation: The CDC reports fentanyl is now involved in 80% of overdose deaths, requiring even broader access to naloxone.
Conclusion: A Call to Action for Communities
The opioid crisis is a complex issue, but naloxone represents a tangible solution. By expanding access and prioritizing education, communities can save countless lives. However, this effort requires collaboration—between policymakers, healthcare providers, schools, and individuals. As one public health official put it, “Naloxone is a bridge to treatment, not an endpoint. We must build it together.” Whether it’s advocating for policy change, attending a training workshop, or simply learning how to use naloxone, every action contributes to a safer future.
Resources
- Where to Get Naloxone: Locate nearby distribution sites at CDC’s Naloxone Finder.
- Training Programs: Explore free online courses at OpioidUniversity.org.
- Advocacy: Join the Naloxone Access Now Coalition to support policy change.
By working together, we can turn the tide against the opioid crisis, one life at a time.

[…] Needs: Do you require family therapy, trauma-informed care, or bilingual […]
[…] fentanyl or other opioids are suspected, use naloxone (Narcan) as a nasal spray or injection. Note: Naloxone is ineffective for non-opioid […]
[…] Can naloxone save someone from a M30 pill overdose?Yes, naloxone can rapidly reverse the effects of fentanyl. However, it may not keep the person […]